Breast cancer is the most common cancer among women in Singapore – and in the world. Many of us will know someone who’s been affected by it; a family member, friend or colleague. That’s why it’s worth going for regular check-ups to ensure that you’re okay, particularly if you have a family history of the disease. Early detection can do wonders. The team at Pacific Prime tells us about the importance of screenings, the issue of treatment costs, and how critical health insurance can help.
How is breast cancer detected?
According to the Singapore Cancer Registry, the incidence of breast cancer diagnoses in women (age-standardised rates) has been increasing since 1975. The likelihood of developing the cancer includes factors such as age and family history. Since early detection can improve survival chances, you should get screened on a regular basis – especially if you’re 50 or over.
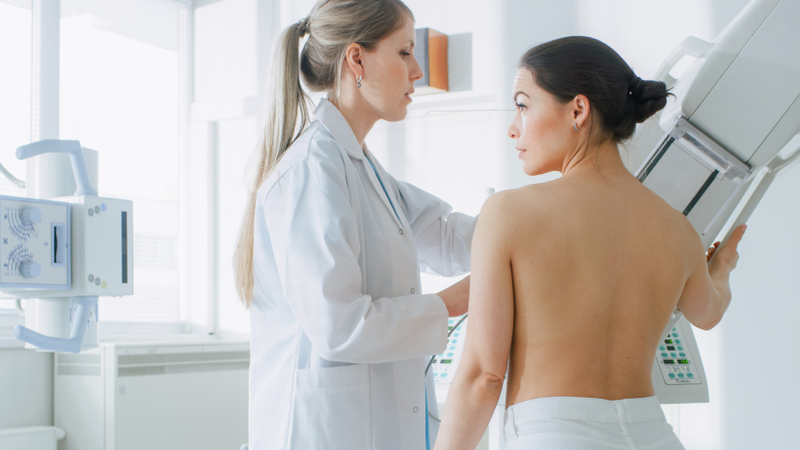
Mammograms are currently the best screening tool. They can’t prevent cancer, but they’re helpful in detecting cancer in its early stages. (Earlier-stage cancers can be treated without mastectomies.) But they’re not flawless. In some cases, cancer can hide in normal breast tissue. And sometimes an abnormality may look like cancer, but it ends up being normal. Knowing these limitations, it’s worth learning how to do regular breast self-examinations and going for routine examinations by a healthcare professional. Occasionally, other types of breast imaging such as an MRI, breast ultrasound or 3D mammogram may be used.
How much does breast cancer treatment cost?
It can be expensive. Costs not only include multiple rounds of chemotherapy treatments; you also might need surgery, follow-up scans or consultations with doctors. According to the Ministry of Health, the costs start from $5,000 for surgery at private hospitals, excluding chemotherapy and other treatments.
What can I do to ease the financial burden?
First of all, ensure you have a good hospitalisation insurance policy. This offers coverage for your hospitalisation charges, including chemotherapy and the cost of surgery. If you’re a Singaporean or Permanent Resident, MediShield Life will help to cover costs for Class B2 and Class C wards. Those who’d rather stay in a Class A or Class B1 ward will need to have an integrated shield plan for coverage.
It’s recommended to get a whole or term life policy that has a critical illness component, in case you’re diagnosed with any of the covered illnesses. Breast cancer is usually included in the list. Read your policy carefully to get a full understanding of the definitions and stages of the illnesses covered, along with payout details.
Is critical illness insurance still necessary?
Some people ask, “If I already have hospitalisation insurance, do I still need a critical illness plan?” What sets hospitalisation and critical illness coverage apart is the way the coverage works. A hospitalisation insurance plan will allow you to claim hospitalisation fees. On the other hand, critical illness coverage enables you to claim the amount assured (depending on the stage of illness) upon diagnosis. You’ll get a lump sum payment, which you can then use at your own discretion.
So having critical illness insurance will give you more freedom in how you choose to use the lump sum payout. For example, you can use it for post-operative treatments, supplementary medical expenses or even for daily living as you recover.
So, what type of plan should I get?
It depends on many factors such as your health, family medical history and budget. A standard critical illness insurance policy may be sufficient for some, but it’s worth considering a plan with extra coverage. If you already have health insurance in Singapore, you may want to add critical illness insurance onto your existing policy, instead of buying an entirely new one. Check with your insurer or broker to find out if breast cancer insurance cover and pre-existing condition cover are included in your plan.
You can also contact the team at Pacific Prime Singapore for more advice, or visit their website to get a free quote.
Written in collaboration with:
Pacific Prime Singapore
18 Cross Street, China Square Central, #14-05
6346 3781 | pacificprime.sg
Read on for more health topics in Singapore:
Dengue fever in Singapore: All you need to know
Does insurance cover alternative medicine?





