A diagnosis of breast cancer in Singapore is no longer as bleak as it used to be. DR OOI WEI SEONG talks us through some common breast cancer causes, symptoms, where to have a biopsy and available treatments like a mastectomy.
Between 2015 and 2019, some 78,824 cancers were diagnosed in Singapore, often with the help of a biopsy. Breast cancer, the most common among women worldwide, added up to 11,805 cases, or 29.4% percent. Breast cancer occurs in just one percent of men suffering from cancers.
Breast cancer arises from the ducts and lobules in the breasts where milk is produced. Other cancers such as sarcoma and lymphoma can also affect the breasts but these are not strictly breast cancers and are treated differently.

Breast cancer causes and risk factors include gender, ageing, a history of breast conditions requiring biopsies, family history and prior radiation exposure. Other breast cancer causes include obesity, early menstruation, late menopause, alcohol consumption and hormone replacement therapy.
Around five to 10 percent of breast cancers arise when the patient has inherited a mutated gene, BRCA1 and BRCA2 being the most common.
Biopsies & cancer symptoms
Unlike other cancers, breast cancers tend to get diagnosed with a biopsy in earlier stages, thanks to national screening programmes. These include mammography for women above 50 years old every two years. In some cases, doctors may recommend mammography from the age of 40.
The Singapore Health Promotion Board and its partners conduct annual breast cancer awareness campaigns and on-the-ground activities, as well as reach out to women via social media. These activities have heightened breast cancer awareness amongst women and the importance of noticing any changes to their breasts from one month to the next.
Breast cancer symptoms may include a palpable lump, changes in size or shape, overlying skin described as dimpling, or a newly inverted nipple that points inwards or appears flat.
A biopsy will confirm the diagnosis and identify the subtype of breast cancer. The presence or absence of certain markers from the biopsy, such as oestrogen receptor, progesterone receptor and Her2 gene, will dictate the treatment regime.
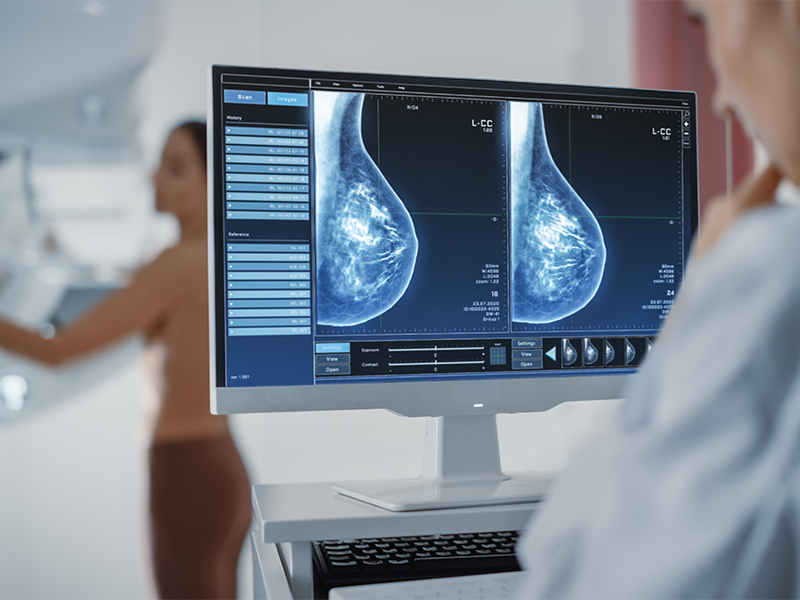
Treatment today: mastectomy or lumpectomy
It is recommended that early-stage breast cancers be removed surgically. Whether the patient receives a lumpectomy or mastectomy depends on the size of the tumour, its location, and whether it has one or more nodules.
The lymph nodes in the armpit on the same side will also be tested. If there is cause for concern, these will also be removed in the same operation.
What happens after a mastectomy?
Following the surgery, a few different modalities of treatment can be used to reduce the risks of recurrence. These include chemotherapy, hormone therapy, radiation and targeted therapy.
The entire treatment may last for a year or longer. For example, a patient with the Her2 gene will need up to a year’s treatment of Herceptin, a drug that blocks the gene, via three weekly infusions. Patients with oestrogen receptor in their tumours may have to take a tablet for between five and 10 years.
The cure rate for breast cancer in Singapore is high, due to early detection, surgical advances and the availability of more medicines that reduce the risks of recurrence.
Breast cancer survivorship often includes the need to monitor and manage the consequences of treatment such as infertility and menopause. Support groups go a long way to ease the shock and trauma of breast cancer, and can be a source of hope and comfort during the worst of the treatment. ICS works with trusted partners to provide support groups for patients.
International Cancer Specialists
#15-01/02 Paragon Tower 1, Lobby F, 290 Orchard Road
6235 9005 | icscancer.com
This article first appeared in the February 2023 edition of Expat Living. You can purchase the latest issue or subscribe, so you never miss a copy!
To make the most of living in Singapore, read our latest City Guide here for free!





