Here’s how your parent’s hip fracture may affect your own health, and what you can do to reduce your risk of brittle bones, bone fractures and even prevent osteoporosis in the first place.
Osteoporosis is an age-related condition characterised by low bone mass and the deterioration of bone tissue. The bones become more porous and brittle (brittle bones), ultimately leading to increased susceptibility to fractures. This includes fragility fractures – bone fractures sustained with minimal force; for example, falling from a standing position.

DR ADRIAN LAU is a specialist orthopaedic surgeon at Hip & Knee Orthopaedics. The Novena-based clinic provides a comprehensive range of screenings and treatments for a range of orthopaedic conditions.
The problem, he says, is that osteoporosis is usually “silent”. Sometimes, there are subtle symptoms such as loss of height and a stooped posture as asymptomatic vertebral fractures occur. However, individuals are usually unaware that they have osteoporosis until they have suffered a bone fracture.
If left untreated, osteoporosis can lead to brittle and fragile bones, which means the bone fractures more easily. It’s often in the wrists, hips and spine, which can severely affect mobility and patient independence.
“In fact, a significant proportion of patients with hip fractures are not able to regain independent living even after successful treatment of those fractures,” says Dr Lau. “That’s why it’s important to reduce fracture risk.”
The good news is that there are steps you can take to assess and actively reduce your fracture risk, and even help slow or prevent bone loss altogether. Here are four of them.

#1 Know if osteoporosis runs in your family – and other risk factors
Individuals who have sustained a previous fragility fracture are at higher risk of sustaining additional fractures. And, those with a family history of osteoporosis are at increased risk of developing osteoporosis and sustaining fractures down the line, particularly as they age. What’s more, osteoporosis is more common in women, particularly post-menopausal women. In fact, the condition affects almost 20 percent of females over the age of 50. Recognising your risk can go a long way in fracture prevention, as it allows for earlier treatment and the appropriate lifestyle changes to be adopted as early as possible. Here are some other risk factors for osteoporosis to be aware of:
- low body weight or being underweight
- height loss (over 2cm) over the course of a few years
- early menopause (before 45 years old)
- certain medications such as corticosteroid use
- low calcium intake (less than 500mg per day)
- excessive alcohol intake (more than two units per day)
- smoking
- a sedentary lifestyle or prolonged immobility
#2 Get your bone health assessed
Fortunately, screening is simple and can effectively determine just where you stand in terms of bone health, says Dr Lau. He recommends it for post-menopausal women, men over the age of 65 and individuals with any of the above risk factors.
Bone health screening usually includes a bone density scan, along with blood tests.
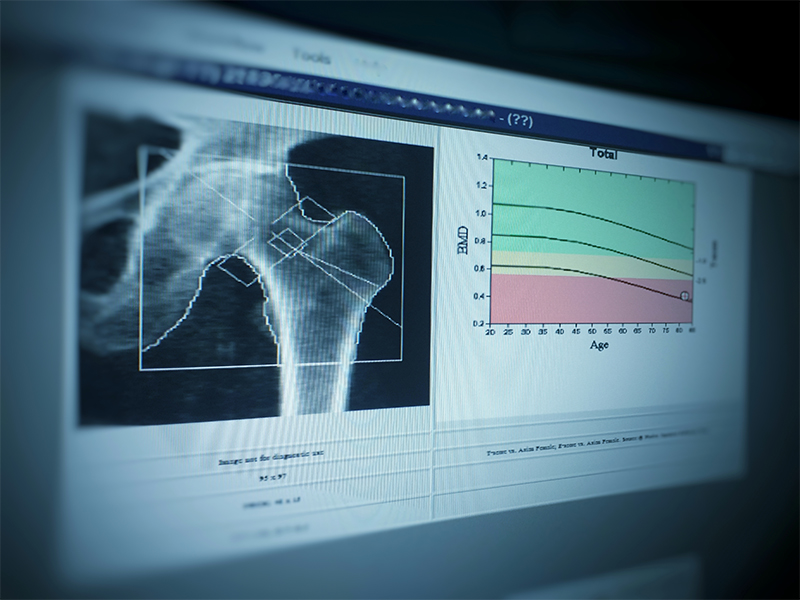
“The bone density scan is a non-invasive, low dose x-ray to measure the mineral content of bone in certain areas of the skeleton. This scan should be done as a baseline, then repeated every one to two years.”
Patients with a T-score (the measure of your bone density compared to that of a person in the peak of their physical condition) of less than or equal to -2.5, and high-risk patients with T-scores of more than -2.5 but less than -1, may be started on anti-osteoporosis treatment. This may include certain medications, along with regular exercise, and a diet rich in calcium and vitamin D.
#3 Make strong bones
Adopting a healthy lifestyle is key to warding off osteoporosis or slowing bone loss in those already living with osteoporosis. “Weight-bearing exercise such as strength training, walking and jogging can help build and strengthen bones,” explains Dr Lau.
“You can also support bone health by ensuring that you’re getting enough calcium and vitamin D in your diet.” He recommends post-menopausal women and men over the age of 70 get at least 1300mg of calcium per day. While dairy has the highest level of calcium, other rich sources include sardines, spinach and almonds. He also advises limiting caffeinated drinks as caffeine (and high acidity) can affect calcium absorption.
#4 Accident-proof your environment, where possible
Reducing the events that could lead to potential hip fractures is important for individuals with osteoporosis, and those patients who do not yet have osteoporosis but are at increased risk of fractures. Dr Lau suggests installing night lights, grab bars in bathrooms and anti-slip mats, and removing any would-be floor obstacles. He also recommends a “visual acuity evaluation” to reduce any sight-related mishaps.
With appropriate treatment of osteoporosis, and optimisation of the various factors to reduce fracture risk, we can slow bone loss, and reduce the events that lead to bone fractures.
Hip & Knee Orthopaedics
#09-21/38 Mount Elizabeth Novena Specialist Centre, 38 Irrawaddy Road
8884 1642 | hipkneeortho.com.sg
This article first appeared in the July 2023 edition of Expat Living. You can purchase the latest issue or subscribe, so you never miss a copy!
To make the most of living in Singapore, read our latest City Guide here for free!
Don't miss out on the latest events, news and
competitions by signing up to our newsletter!
By signing up, you'll receive our weekly newsletter and offers which you can update or unsubscribe to anytime.

