Bid farewell to festive indulgences and say hello to a fitter and stronger body! How? By scheduling one of these effective body-shaping, body-sculpting and body-contouring slimming treatments. Here are some top recommendations from Singapore’s aesthetic doctors and therapists, offering a variety of technologies and services to address any niggling issue.
Bye-bye fat with body-shaping Emsculpt Neo
If you’re looking to tone up your bod in 2024 – even the ever-problematic areas such as soft abdomens, flabby arms, sagging buttocks and weak calves – you might want to look into Emsculpt Neo at Dr KW Chan Clinic.
Following its predecessor Emsculpt, Emsculpt Neo is a groundbreaking body-shaping and body-sculpting technology in the beauty world. It’s the only non-invasive technology that simultaneously uses radiofrequency and HIFEM+ (high-intensity focused electromagnetic field) to eliminate fat and build muscle. As such, Dr Chan and his team are able to achieve more fat destruction and muscle growth with this combined technology than any other typical device.

How does it work? This slimming treatment sees HIFEM+ energy contracting muscle fibres in the treated area at intensities unachievable during a normal workout. Extreme stress forces the muscle to adapt, resulting in hypertrophy and hyperplasia. Due to radiofrequency heating, in less than four minutes the temperature in the subcutaneous fat reaches levels that cause apoptosis. This is where fat cells are permanently damaged and slowly removed from the body.
The slimming treatment is suitable for men and women with BMIs up to 35. Clinical studies have reported on average an impressive muscle volume increase by 25 percent and a 30 percent reduction in subcutaneous fat, with results maintained for up to an impressive six months post-treatment.
#02-19/20 OUE Downtown Gallery Tower 2, 6A Shenton Way
6011 1630 | WhatApp: 9654 9863 | drkwchanclinic.com
A triple-threat body-shaping and body-contouring slimming treatment
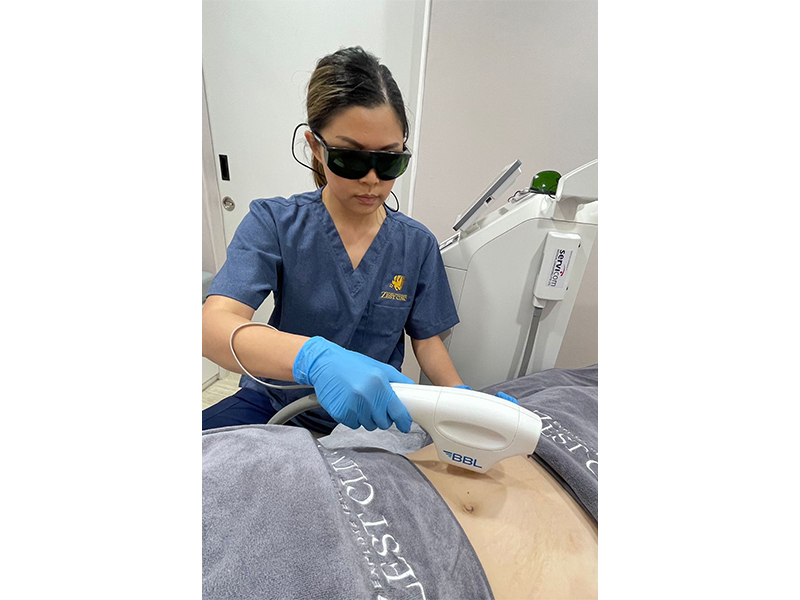
At Zest Clinic, you’ll find a range of health and aesthetic slimming treatments designed by co-founders Dr Sankeerth Reddy and Dr Tiffany Yeo-Reddy to take your wellbeing and fitness to the next level. At the top of the list is its signature Firm and Tone. It’s a cutting-edge triple modality treatment consisting of laser tightening, radiofrequency and magnetic pulse therapy.
This triple threat involves devices like FOTONA Dynamis, Sciton BBL Body and Venus Legacy to melt skin fat and improve skin laxity through collagen tightening on areas like the belly, flanks, arms, thighs, buttocks, back, neck and chin. The best part? There’s minimal downtime post-treatment, which means no disruption to your busy lifestyle. It’s not just about quick fixes either. The Zest Clinic team makes it a priority to guide clients through true weight loss and body composition change with tailored medical treatments like Saxenda, Ozempic, Wegovy and Rybelsus.
It also offers functional nutrition programmes based on individual metabolism and genetics. There’s even AI-based nutrition and fitness support as well as on-demand tele-consultations that can suggest and tailor recommendations to clients, guiding them through long-term lifestyle modifications beyond the clinic. Get ready for a fitter, firmer and more fabulous you this 2024!
#01-11B Parkway Parade, 80 Marine Parade Road
9176 9378 | IG: @zestclinic.singapore | zest.clinic
Contour your body with BaySculpt EMS slimming treatment
Achieving your dream body has never been easier thanks to the latest advancements in non-invasive body contouring treatments you can find right here in Singapore. Case in point? The BaySculpt Electromagnetic Stimulation (EMS) available at Bay Aesthetics Clinic. This non-invasive, zero-downtime body contouring treatment focuses on engaging skeletal muscles to trigger cascades of contractions. This helps to build up the muscles of the abdomen, buttocks, inner thighs and arms, while burning fat. It’s also effective for treating abdominal muscle separation after childbirth.
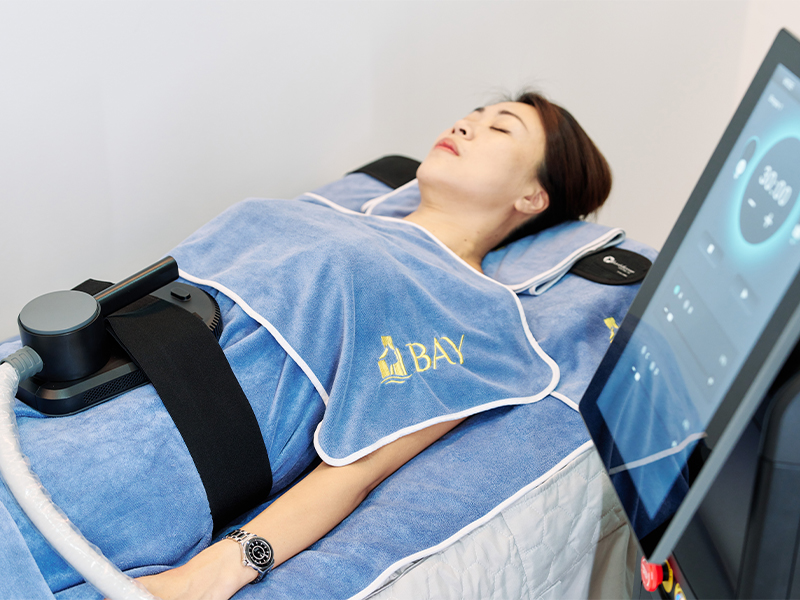
In a 30-minute session, the technology generates 20,000 supramaximal muscle contractions. That’s akin to over 20,000 crunches! At the same time, the discomfort level is minimal. While the contractions may feel like muscle cramps at first, your body will get accustomed to it. You’ll experience mild muscle soreness afterwards. For the best results, it’s recommended to undergo ten to twelve sessions, twice a week. Visible transformations can be expected within two to three months. With regular sessions, the BaySculpt EMS can boost muscle hypertrophy for larger muscles while breaking down fat deposits. This helps to banish stubborn fat, tighten loose skin and enhance overall body shape.
#B2-12 Marina Bay Link Mall, 8A Marina Boulevard
8428 7811 | | FB: @bayclinicsg | IG: @bay.clinic | bayclinic.sg
Build muscles in minutes with Magneat FMS
Are you after lean, toned muscles but aren’t a fan of slaving away for hours in the gym? We don’t blame you! Thankfully, Magneat FMS (functional magnetic stimulation) is a 15-minute body-shaping and body-sculpting muscle toning treatment at Chez Moi De Beaute that can help strengthen your tummy muscles, sculpt your glutes, or perk your butt while you laze on a plush bed.
Magneat FMS utilises a static magnetic field equivalent to 1.8 teslas to stimulate motor nerves in muscles for a deep exercise effect. What makes it unique is that its penetration reaches your deep core muscles at up to 10 centimetres. This allows it to develop a stronger body from the inside out. There’s also no radiation, heat or electrical current transmitted. You may feel muscle contractions on your targeted area and soreness post-treatment, much like after a strenuous workout.
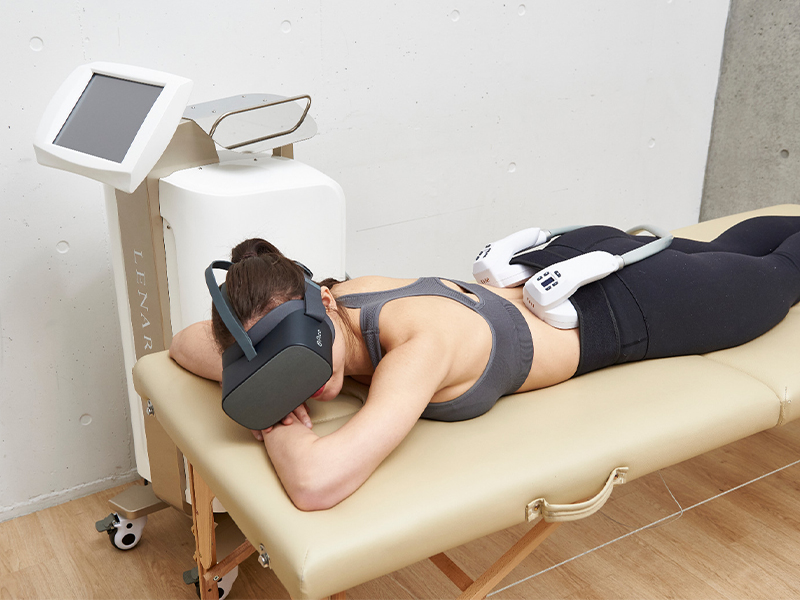
It’s effective in toning muscles, improving posture and increasing basal metabolic rate even when resting, thus complementing weight loss. It’s also great for sufferers of diastasis recti and urinary incontinence as it can quickly strengthen and rebuild rectus abdominus and pelvic floor muscles. One or two sessions weekly is recommended. Noticeable improvements can be seen after one to three sessions, and stable and visible results in 12 weeks. Try a 15-minute session now at the special price of $68!
#01-91/92 Far East Plaza, 14 Scotts Road
Call/WhatsApp: 8721 8123 | chezmoi.com.sg
Sculpt and Tone with Cryo-Sculpting Fat Removal
No matter how many sit-ups we do, the truth is that we cannot “spot reduce” fat. In other words, fat from specific problem areas like stubborn tummies and love handles can’t be eliminated through workouts or diets alone! However, the Cryo-Sculpting Fat Removal slimming treatment at 8 Medi-Aesthetics may offer a solution. This body-shaping and body-sculpting treatment freezes excess fat to remove it from stubborn areas in a process called cryolipolysis. The word translates to “cold” (cryo) “fat” (lip) “destruction” (lysis). As fat freezes at higher temperatures than other surrounding skin, it can be selectively frozen while the skin and surrounding tissues are left unharmed. What’s more, the fat lost from fat freezing is lost permanently (as fat cells do not regrow or migrate to other areas of the body), promising longer-term results.
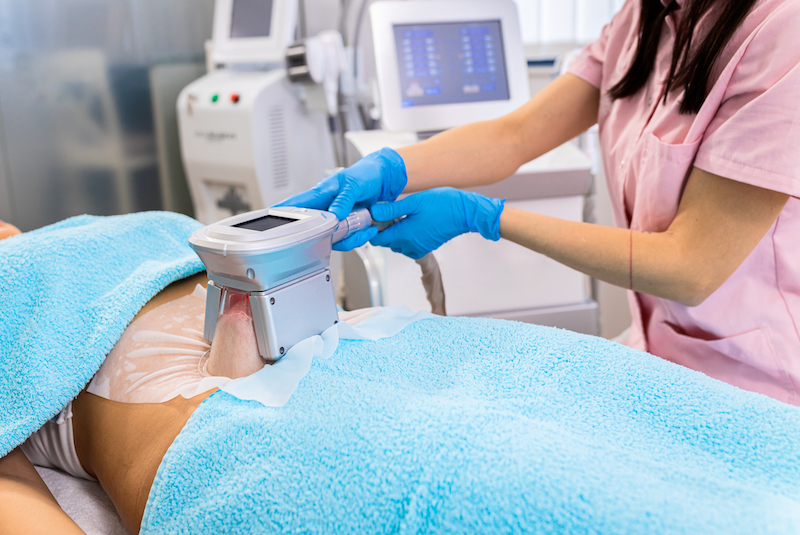
Great for those looking for a safe, effective and non-invasive slimming treatment to contour the body, Cryo-Sculpting Fat Removal can be done on more than one area in a single session. You can expect to lose up to 30 percent of the targeted fat per treatment, with results visible around three weeks after. There’s also zero downtime or recuperation, making this a fantastic slimming treatment for busy ladies and gents.
Head here for locations, or read more about treatments here.
6973 6593 | Whatsapp: 9230 1377 | Booking link
This article about body contouring slimming treatments first appeared in the February 2024 edition of Expat Living. You can purchase the latest issue or subscribe so you never miss a copy!
To make the most of living in Singapore, read our latest City Guide here for free!