If you’re wondering “Why won’t my tummy go away after pregnancy?” months after giving birth, you may have abdominal separation, or diastasis recti (DR). But, how do you know if you have DR? And can it improve without surgery? Here, a top women’s physio in Singapore who specialises in this area shares how to fix abdominal separation.
What causes abdominal separation?
Abdominal separation can develop before, during or after pregnancy.
The connective tissue (linea alba) thins out in response to a mother’s hormonal changes, expanding uterus and an increase in intraabdominal pressure. As a result, the space between the left and right tummy muscles widen, creating a gap. In many cases, the tissues get so stretched during pregnancy that they lose their elasticity – that is, the ability to retract back into position (like an overstretched rubber band) after pregnancy. When put under pressure, the abdominal walls can’t hold together. Organs including the intestine, bladder or uterus can be felt or seen bulging through the thinned and separated abdominal muscles. This can cause a tummy bulge that just won’t go away.
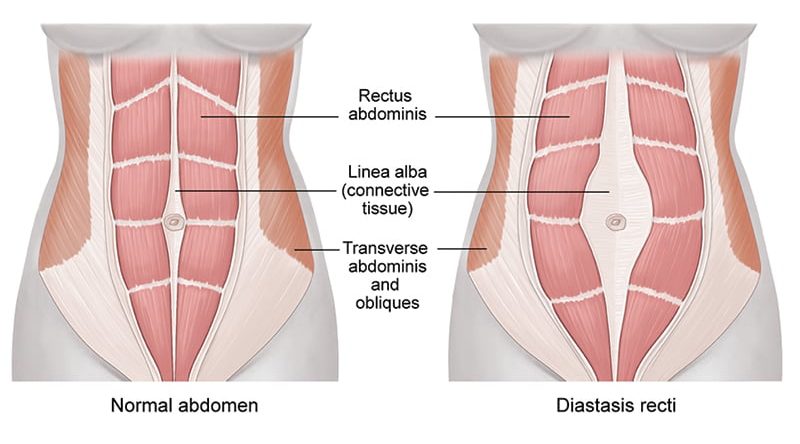
Many mums worry most about having a gap. But, it is not actually the gap itself that causes the protruding tummy. It is more the lack of core stability and strength holding everything back.
Being of older age and having multiple pregnancies, twins or triplets, or babies with a high birth weight can increase likelihood of the severity of abdominal separation and recovery potential. But, abdominal separation often occurs in single baby pregnancies – and it can happen to anyone.
A protruding “mummy tummy” isn’t the only side effect. For some, it can cause lower back pain, incontinence (uncontrolled weeing), a lack of core strength, pelvic floor dysfunction and poor posture. In some instances, an umbilical hernia occurs; the intestine or other tissues bulge through the weak spot around the belly button, making the belly button stick out permanently.
How do you know if you have abdominal separation?
Trained physiotherapists experienced in seeing women after birth can examine your muscles and assess the severity of the damage to your connective tissue.
BEX ALDRIDGE is a top trainer and physio in Singapore. As a mum herself, Bex knows first-hand just how hard pregnancy and childbirth can be on the body. That’s why she founded Health2mama, which offers physiotherapy, personal training, wellness and postpartum recovery services for mums and babies, during and after pregnancy. (And, conveniently, they come to you!)
All of Health2mama’s trainers are physiotherapists who specialise in seeing mums, so they’re super experienced in dealing with prenatal and postnatal bodies.
“Assessing DR by a professional involves a lot more than just feeling the gap with fingers,” says Bex. “It’s actually the tension that can be generated in your core that needs to be checked, and in different positions. For example, standing and doing certain activities, rather than just in a lying-down position.”
Tape measurements and before-and-after photos are also useful in showing progress, she says.
Other factors that can contribute to DR should be checked, too. These include rib mobility, breathing strategies and pelvic floor strength; also, the strength and flexibility of a number of muscles in the body that are linked to your core.
“Only then can a programme be put together to help you as an individual work on your weaknesses and heal your diastasis recti,” says Bex.
And, the sooner you discover you’ve got DR, the better. “Starting the right exercises early to help heal abdominal separation is key. For instance, it’s much harder to correct, and takes a lot longer, if left more than eight weeks before starting on a rehab programme.”
How to fix abdominal separation
If you’re wondering how to fix abdominal separation, you’ll be happy to know that it’s possible with physiotherapy and the right exercises.
“A women’s physiotherapist trained in treating DR can start you on a safe programme of specific exercises and progress you to harder exercise gradually. This will help the connective tissue to heal and regain its tension, improving stability and strength in your body, and also help close the gap. Health2mama offers a unique online, eight-week Diastasis Healing exercise programme for mums to follow at home, supported by physios.”
Originally designed by Bex to heal her own DR, Health2mama’s Diastasis Healing programme has helped loads of women, showing them how to fix abdominal separation.
There are different DR healing programmes to choose from: an online follow-yourself programme, face-to-face consults, or a combination of both. Regardless of which you choose, the programme helps to:
- build a stronger pelvic floor and core;
- heal the abdominal separation;
- flatten your tummy;
- help with any incontinence;
- improve posture; and
- improve your general tone and strength.
“The main thing that helps to heal a DR is reconnecting your brain to your breathing, abdominal muscle, pelvic floor and glutes, and teaching them to all work together. This helps you get back to the exercise and sports you were safely doing before pregnancy, without causing any harm.”
So, can diastasis recti be fixed without surgery?
Surgery often isn’t necessary. Doing the right DR exercises and working with a women’s physiotherapist can be enough to close the gap and help you regain your core strength. In fact, before considering surgery, Bex and others in the medical field suggest working with a physiotherapist for at least a year, as the first treatment approach.
“If you see improvements over the year, then continue beyond that until there are no further improvements,” she says.
If that doesn’t work – or in the case of a tear – surgical repair may be an appropriate option. In fact, it’s widely done with general and plastic surgeons here in Singapore.
The surgery isn’t just for cosmetic purposes. Since the back and abdominal muscles work together to protect the spine and allow for pain-free and functional movements, a break in this synergistic system can cause lower back pain and pelvic floor muscle dysfunctions such as incontinence, constipation, vaginal pain or pain during intercourse in some instances. Surgery helps bring the muscles closer together, restoring some strength around the core.
If you do opt for surgery, Bex advises strengthening your abdominal, pelvic floor and core muscles beforehand in any case; doing so will help support the sutures and surgery. A pre- and post-surgery rehab programme will allow for a regain in overall core muscle strength and function a lot quicker.
Choosing an experienced women’s physio in Singapore
With abdominal separation, it’s important to work only with a professional who is experienced in working with mums with DR. There are lots of do’s and don’ts when it come to living with DR. A trained women’s physiotherapist will know what’s best for you.
“A lot of articles out there say that planks, ab curls, lifting heavy weights and leg raises are out of the question if you have abdominal separation, but this isn’t true,” says Bex. “With the right rehab programme and support from a professional, you can be shown modifications of these exercises so that you can do them safely. This will actually help your DR to heal and flatten your tummy, rather than make it worse. As you become stronger, the exercises can gradually be made harder, and adding weights and resistance is of benefit to getting the best results. You can then return to lifting heavier weights, and do full planks and leg raises again.”
For more information or to book an appointment with Health2mama, call 6255 5250 or visit health2u.sg/health2mama.
For regular tips and diastasis recti healing workouts, follow @Health2mama
Like this? Read more in our Health & Fitness section and good gyms in Singapore.






